
The NERD Model: Why Some Concussion Patients Get Stuck
If you treat concussion patients long enough, you start to notice a pattern.
Some patients improve steadily. Others don’t, and seem to cycle endlessly. Their symptoms fluctuate, the exam findings are persistent, and recovery never really progresses.
They’re not deteriorating.
They’re not failing treatment.
They’re just ... stuck.
That observation was one of the starting points for the model described in “The NERD Model: Reflex Circuit Dysfunction as a Systems-Level Driver of Persistent Post-Concussion Symptoms.” The goal wasn’t to introduce a new label, but to explain a familiar clinical reality: recovery can stall when the nervous system becomes trapped in maladaptive feedback loops.
The Brain Isn’t Broken ... It’s Looping
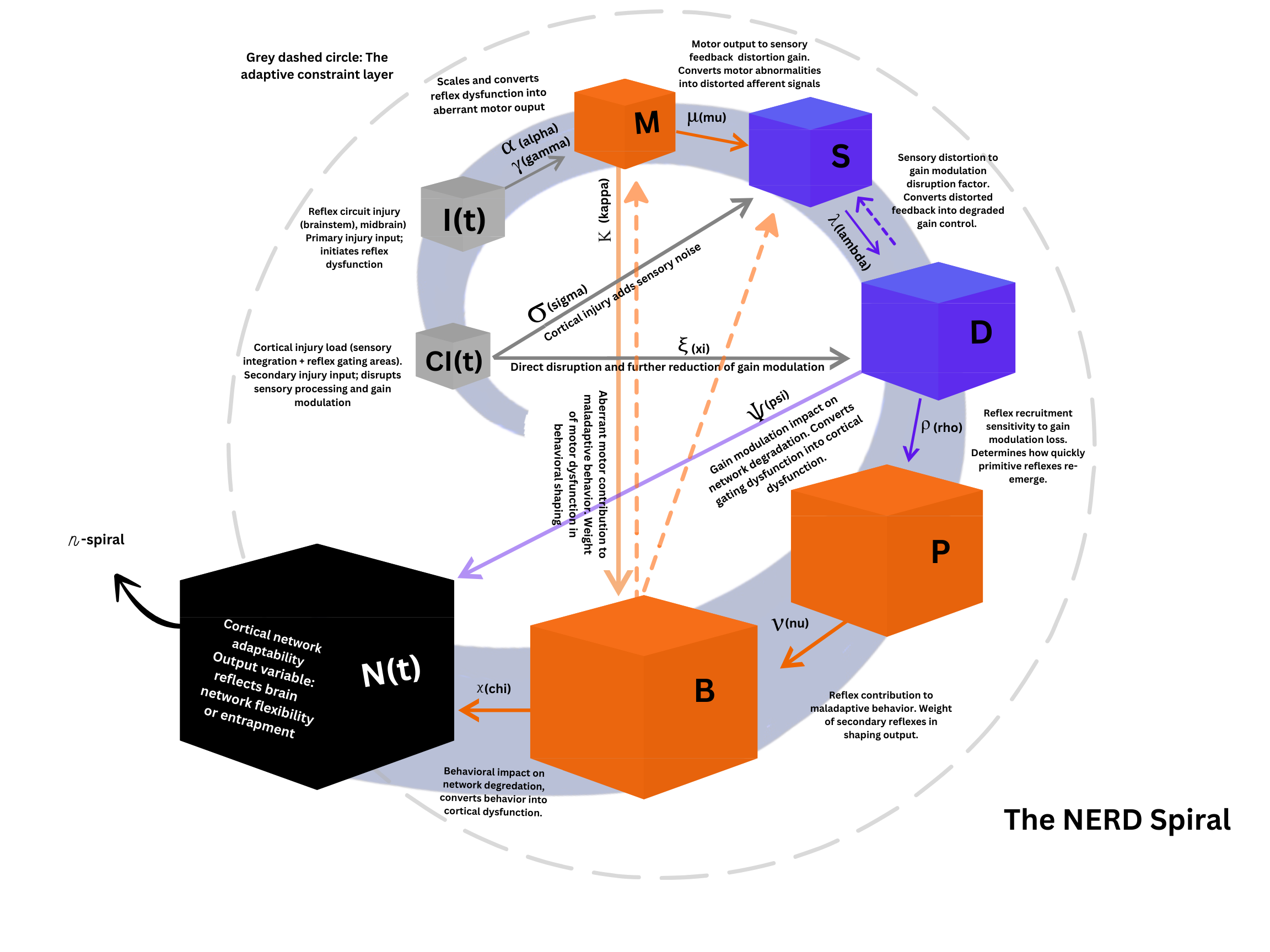
The NERD model (Network Entrapment by Reflex Dysfunction) frames the brain as a hierarchical control system made up of interacting loops rather than isolated parts.
At a simplified level, these loops include:
- Sensory input loops (visual, vestibular, proprioceptive, interoceptive)
- Reflex loops (brainstem-mediated vestibular, postural, ocular, and autonomic reflexes)
- Modulatory loops (cerebellar timing and gain regulation, basal ganglia–thalamic gating)
- Cortical loops (prediction, perception, cognition, and behavioral output)
In a healthy system, these loops continuously update one another. After concussion, one or more of them can lose flexibility. When that happens, the system may repeatedly return to the same functional state—even when interventions are applied.
That’s the “Groundhog Day” problem in clinical form (in reference to the 1993 movie featuring Bill Murray).
A Concrete Example: Vestibular Reflex Dysfunction
Consider a patient with persistent dizziness, visual motion sensitivity, balance issues, neck tension, and cognitive fatigue.
Traditional approaches often localize this to the vestibular apparatus, the cervical spine, or cortical processing. The NERD model asks a different question:
Which loop is failing to recalibrate?
If someone's cerebellum is injured in a concussion, it has been deomstrated that vestibulo-ocular and vestibulo-spinal reflexes are dysregulated. This causes regression of reflex modulation, resulting in distorted orientation signals continue that ascend through the brainstem. The cerebellum, again, to struggles to normalize timing and gain. This results in noisy signals to the thalamus, and failure to gate noisy input to the cortex. The cortex increases effort, vigilance, cognitive load, decreases metabolic efficiency. The cortex then makes "decisions" based on honest, yet inaccurate input (often termed "compensations"), causing further distortion of (in this example) vestibular signals.
In this scenario, dizziness, tension, visual motion sensitivity, balance issues, and fatigue are not the primary problems—they're the signals that the system has lost its ability to normalize and adapt.
Why This Matters Clinically
The practical value of the NERD model is that it shifts the clinical question.
Instead of asking, “What structure is damaged?”
We ask, “Which loop is entrapped, and what input will facilitate normalization of its function?"
This framework is taught explicitly in the Functional Neurology Management of Concussion Program at the Carrick Institute. Clinicians are trained to:
- Identify dominant dysfunctional loops
- Understand how reflex circuits interact with cerebellar and thalamocortical systems
- Apply targeted interventions aimed at restoring adaptability, not just suppressing symptoms
This is not about doing more techniques. It’s about intervening at the appropriate level of system control.
Bridging Old Neurology and Modern Systems Thinking
One of the strengths of this model is that it does not abandon classical neurology. It builds on it.
The idea of hierarchical organization and loss of adaptive control has deep roots in neurological thought, and much of the clinical philosophy underlying this work traces back to my mentor, Ted Carrick, whose career focused on understanding the nervous system as an adaptive whole.
Equally important is the contribution of my dear colleague and co-author, Dr. Kenneth Jay, whose talent in the ability to formalize clinical observations using modern systems and mathematical reasoning strengthens the model and keeps it disciplined and testable.
An Invitation to Think Differently
This paper doesn’t claim to replace existing concussion approaches. It explains why many of them work—and why they sometimes stop working.
If you’ve ever felt like you were doing your best to treat a concussion patient, they make progress only to regress again, the NERD model offers a way to identify what’s keeping the system locked in place—and how to help it move forward.
That's the work. And this is the invitation.
Please read our publication and share with your networks: https://www.frontiersin.org/journals/systems-neuroscience/articles/10.3389/fnsys.2025.1673195/full
The NERD Spiral
These courses provider a Deeper Dive into this topic.
%
Off


Functional Neurology Management of Concussion Level 2
Level 2 of Functional Neurology Management of Concussion moves beyond symptom lists into the network, sensory, and physiological complexities that often hold patients back. With advanced diagnostics, layered rehabilitation strategies, and structured workflows, you'll be ready to resolve barriers that keep recovery from reaching its full potential.
$
/hr.
$
/hr.
$
/hr.
$
/hr.
$
/hr.
$
/hr.
|
hours
More Insights
.png)
BTSP: The Discovery of Instantaneous Neuroplasticity
For a century, neuroscience taught that plasticity meant slow yielding under repeated pressure. A new discovery says otherwise. Behavioral timescale synaptic plasticity — BTSP — shows that the brain can rewire itself in a single moment when two specific signals converge in the right network. Here's the science, and why it offers a long-overdue explanation for what skilled functional neurology providers have been observing in the clinic for decades.

The New "Flexible Access" Policy: Access that Meets Your Needs and Budget
Carrick Institute's Flex Access policy delivers faster course completion, lower costs, and flexible learning that actually works. By replacing Unlimited Access with structured timeframes based on course length, scholars gain the motivation and accountability needed to finish courses while maintaining the freedom to extend or revisit content.
When a Concussion Unleashes Something Deeper
When a concussion doesn’t heal as expected, it may reveal something far deeper. This post explores how traumatic brain injury can unmask hidden tick-borne infections—like Lyme and its co‑infections—through shared pathways of neuroinflammation and immune dysfunction. For clinicians, it’s a call to look beyond “post-concussion syndrome” and recognize emerging research that links persistent symptoms, immune dysregulation, and overlooked infection.

Molecular Hydrogen: A Foundational Therapy for Neurology, Regeneration, and Integrative Clinical Practice
Molecular hydrogen (H₂) is emerging as a foundational therapy for integrative clinics. This small molecule crosses the blood-brain barrier, selectively neutralizes harmful free radicals, and supports mitochondrial function. Safe, inexpensive, and easy to implement, H₂ enhances outcomes for neurorehabilitation, chronic inflammation, and regenerative protocols. Learn how to integrate it into your practice.
You're Being Rewired by the World’s Most Popular Recreational Drug—and It’s Not What You Think
Think you know caffeine? Wait until you uncover what it's really doing to your striatum, your thalamus, your sleep pressure system, and even your cholinergic memory circuits. The truth is more complex—and more important—than you've ever been told.

What Healthcare Can Learn From Boy Scouts: An Opinion Piece
We believe that education should be democratized—not locked behind professional guilds or lifetime specialties. That's why we allow any licensed health care provider to take our programs.We may not be able to certify every provider to perform every procedure—regulatory and scope-of-practice rules exist for good reason—but we can provide the knowledge, skills, and frameworks to broaden their thinking and improve their care. When a physical therapist understands neurochemistry, or a medical doctor understands vestibular rehabilitation, patients win.

Diplomate vs. Fellowship in Functional Neurology: The Difference and Why It Matters
Diplomate or Fellow? One proves you’re qualified. The other proves you’re exceptional. In functional neurology and beyond, these two credentials are often confused—but understanding the difference can define your credibility, impact your scope, and elevate your career. This post breaks it down simply, clearly, and with legal clarity every healthcare professional should know.

Why Elite Healthcare Providers Are Mastering Integrative Health
The future belongs to providers who refuse to be limited by traditional boundaries. Master the integration, lead the evolution.
Functional Neurology: The Original Blueprint for Understanding the Dynamic Brain
Discover how functional neurology is transforming patient care worldwide. This post explores the origins of the movement pioneered by the Carrick Institute, its groundbreaking network model of brain function, and how clinicians use these principles to help complex cases that defy conventional treatments. From recalibrating sensory inputs to mastering dynamic brain interventions, learn why thousands of healthcare providers have embraced functional neurology to deliver life-changing outcomes.

Functional Neurology: Rethinking How We Approach the Nervous System
Functional neurology is redefining how clinicians approach neurological dysfunction—seeing the nervous system as a dynamic, adaptable network instead of a static circuit. This article explores its origins, the network model that maps brain function hierarchies, and how targeted interventions recalibrate maladaptive patterns. Learn how this revolutionary systems-based approach helps patients with persistent symptoms and why it’s becoming an essential paradigm for healthcare providers worldwide.
Ready to bring Carrick Institute to your event?
Use the form below to tell us about your organization, audience, and goals. Our team will follow up with availability and speaker recommendations.
Get new articles delivered to your inbox
Stay updated on the latest in clinical neuroscience education—new articles, course releases, research spotlights, and more.
No spam. Just thoughtful content from Carrick Institute faculty and contributors.
.png)
